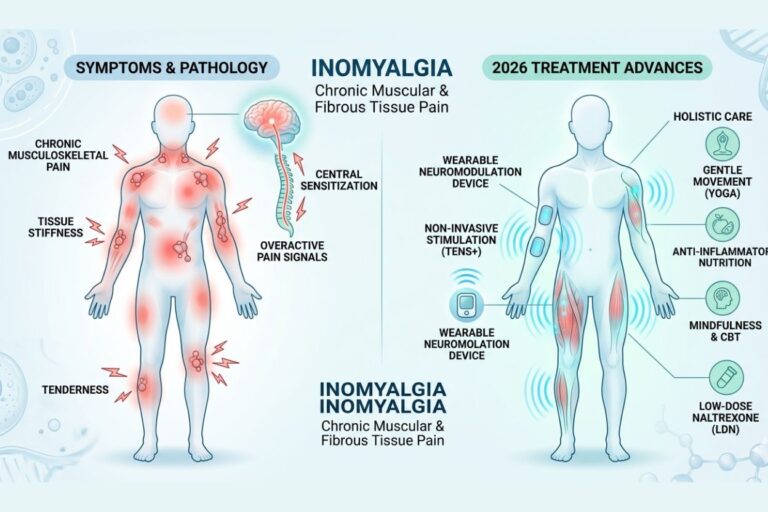
Inomyalgia remains one of the most complex challenges in modern medicine. While often grouped with fibromyalgia, the specific term inomyalgia emphasizes the localized pain within the fibrous tissues and muscles. As we navigate through 2026, scientific breakthroughs have transformed this condition from an “invisible illness” into a well-defined neurological and muscular disorder.
Understanding the nuances of this condition is essential for anyone seeking relief. This guide provides the latest research, diagnostic updates, and human-centric strategies to manage the persistent ache and fatigue associated with fibrous tissue discomfort.
Defining Inomyalgia in the Modern Era
To truly grasp what inomyalgia is, we must look at its linguistic and medical roots. The term is derived from “ino” (fiber), “myo” (muscle), and “algia” (pain). Unlike standard muscle soreness, this condition involves a chronic, systemic amplification of pain signals.
In 2026, researchers clarified the distinction between general fatigue and the specific musculoskeletal distress of this disorder. It is now widely recognized as a nociplastic pain syndrome. This means the pain is real, but it is caused by the way the central nervous system processes sensory input rather than a visible injury to the tissue itself.
Latest 2026 Symptoms and Warning Signs
The symptoms of inomyalgia often fluctuate, making them difficult to track without a professional framework. However, several core indicators have remained consistent in clinical studies this year.
Widespread Musculoskeletal Aching
The primary symptom is a deep, consistent ache that affects both the upper and lower body. Patients often describe the sensation as “having the flu for months.” This pain is typically worse in the morning and can be exacerbated by both intense activity and prolonged periods of rest.
The Rise of Cognitive “Fog”
New data from 2026 highlights the severity of “ino-fog,” a cognitive impairment that affects memory and processing speed. This isn’t just simple forgetfulness; it is a profound mental exhaustion that makes focusing on complex tasks nearly impossible. Recent studies suggest that this fog is directly linked to the brain’s constant effort to “filter out” background pain signals.
Breakthrough Causes: Why Inomyalgia Occurs
One of the biggest questions in medicine has been the “why” behind chronic pain. In 2026, we will finally have clearer answers involving genetics, neuro-inflammation, and the gut-brain axis.
Genetic Predisposition and Triggers
We now know that certain individuals carry specific gene variations that make their nervous systems more reactive. However, these genes usually require a trigger to become active. These triggers can include:
- Physical Trauma: Such as a car accident or a severe fall.
- Viral Infections: Certain long-term viral responses can jumpstart chronic pain pathways.
- Emotional Stress: High-cortisol environments can physically rewire pain receptors over time.
Small Fiber Neuralgia Discoveries
A major breakthrough in 2026 was the discovery of “small fiber neuralgia” in a subset of patients. Researchers have found that some people with inomyalgia actually have hyperactive small nerve fibers that send “fire” signals to the brain without a stimulus. This discovery is revolutionary because it moves the diagnosis from purely psychological to a measurable neurological event.
2026 Diagnostic Protocols: No More Guessing
In the past, patients would spend years visiting different specialists before receiving a name for their pain. Today, the diagnostic process for inomyalgia is faster and more accurate.
Moving Away from Pressure Points
While the old “18 tender points” test is still known, the 2026 protocols prioritize the Widespread Pain Index (WPI) and the Symptom Severity (SS) scale. Doctors now look at the total “pain load” on the body and how much it interferes with daily life, sleep, and mood.
AI-Assisted Diagnosis
Artificial Intelligence has entered the clinic. New AI models can now analyze a patient’s self-reported pain patterns and compare them against thousands of global cases. This allows for an earlier diagnosis, often within the first six months of symptom onset, which is crucial for long-term management.
Advanced Treatment Strategies for 2026
Treatment for inomyalgia has shifted from “managing symptoms” to “re-training the nervous system.” A successful plan in 2026 is always multimodal, combining technology with lifestyle changes.
Non-Invasive Neuromodulation
One of the most effective tools used today is TENS (Transcutaneous Electrical Nerve Stimulation) integrated with physical therapy. Recent clinical trials in 2026 proved that using TENS for just 30 to 60 minutes a day significantly reduces movement-evoked pain. This allows patients to stay active without the usual “flare-up” that follows exercise.
Pharmacological Innovations
While older medications like duloxetine are still used, 2026 has introduced low-dose naltrexone (LDN) as a popular alternative. LDN works by briefly blocking opioid receptors, which then triggers the body to produce more of its own natural “feel-good” endorphins. This helps dampen the overactive pain response without the side effects of traditional painkillers.
The Vital Role of Nutrition and the Microbiome
We cannot discuss inomyalgia without mentioning the gut. New research shows a direct link between gut health and pain sensitivity. An imbalance in gut bacteria can lead to “leaky gut,” which allows inflammatory markers to enter the bloodstream and irritate the nervous system.
Anti-Inflammatory Eating Patterns
In 2026, the “Ino-Diet” gained traction. This involves:
- High Omega-3 Intake: Found in walnuts, flaxseeds, and fatty fish to soothe nerve inflammation.
- Eliminating Processed Sugars: Sugar is a primary trigger for muscle stiffness and energy crashes.
- Magnesium-Rich Foods: Spinach, almonds, and dark chocolate help relax muscle fibers and improve sleep quality.
Mental Resilience and the Power of CBT
The psychological burden of chronic pain is immense. However, research in 2026 has shown that the brain is plastic—it can be changed. Cognitive Behavioral Therapy (CBT) remains a gold standard because it teaches the brain to “de-catastrophize” pain.
When you stop fearing the pain, the body’s stress response lowers. Lower stress means lower cortisol levels, which ultimately lead to fewer pain signals. This virtuous cycle is the key to long-term remission. Many patients now use digital health apps to practice these CBT techniques from the comfort of their homes.
Lifestyle Adjustments: Thriving with Inomyalgia
Living a full life with inomyalgia is entirely possible with the right adjustments. The goal is to live “with” the condition rather than constantly fighting against it.
The Art of Pacing
Pacing is the most important skill for a patient to learn. It involves doing small amounts of work followed by planned rest, even if you feel “good.” Overexertion on a good day often leads to a “crash” the next day. By staying within your “energy envelope,” you can maintain a steady level of activity throughout the week.
Sleep Hygiene Breakthroughs
Since sleep is when the body repairs fibrous tissues, it is a top priority. In 2026, specialized “cool-touch” bedding and weighted blankets have become standard recommendations. These tools help regulate body temperature and provide a grounding sensation that calms the nervous system, enabling deeper, more restorative sleep.
Summary of the 2026 Outlook
The landscape for inomyalgia has never been more promising. We have moved from a place of confusion to a place of high-tech, human-centered care. With the integration of AI diagnostics, wearable nerve stimulators, and a deeper understanding of the gut-brain connection, the “invisible” pain is finally being seen and treated effectively.
If you or a loved one is struggling with these symptoms, remember that you are not alone. The medical community now has the tools to help you reclaim your vitality. By staying informed on these 2026 updates, you are already taking the first step toward a pain-free future. Stay consistent with your movement, mindful of your nutrition, and gentle with your mental health. Success in managing inomyalgia is a marathon, not a sprint, and every small victory counts.